MRSA Care Guide
from the CDC Pocket Guide to MRSA and the CDC website
MRSA Infection
Staphylococcus aureus (S. aureus), also known as staph, is a common bacterium found on the skin or in the noses of up to 30% of healthy people in the United States. These people are called “carriers”; they usually do not know they carry the bacterium and never get sick from it. The bacteria are harmless unless they penetrate the body’s natural barriers and cause infection. Staph can cause a wide range of infections that affect the body, both internally and externally, and are the most common cause of skin and soft tissue infections in the United States. Staph can occasionally spread rapidly into the bloodstream and, if untreated, can cause death. Although risk factors for transmission of MRSA are not clear, incarcerated populations may be more susceptible to MRSA infection due to conditions such as:
Staphylococcus aureus (S. aureus), also known as staph, is a common bacterium found on the skin or in the noses of up to 30% of healthy people in the United States. These people are called “carriers”; they usually do not know they carry the bacterium and never get sick from it. The bacteria are harmless unless they penetrate the body’s natural barriers and cause infection. Staph can cause a wide range of infections that affect the body, both internally and externally, and are the most common cause of skin and soft tissue infections in the United States. Staph can occasionally spread rapidly into the bloodstream and, if untreated, can cause death. Although risk factors for transmission of MRSA are not clear, incarcerated populations may be more susceptible to MRSA infection due to conditions such as:
- Overcrowding
- Higher prevalence of mental illness, hindering efforts to improve hygiene
- Greater prevalence of MRSA colonization in those within the facility
- Injection drug use
- Immune system depression
Because of this susceptibility, correctional facilities can serve as amplifiers of MRSA skin disease.
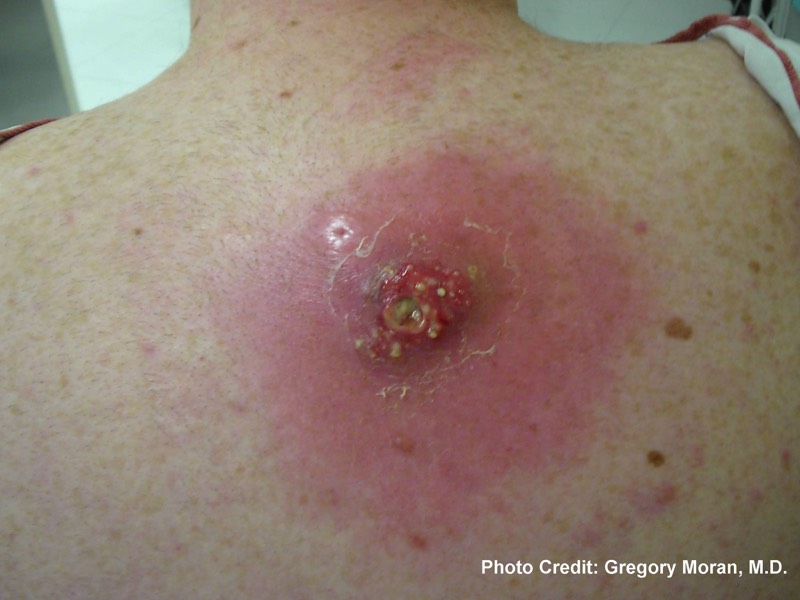
Identification
Recognition:
Identification of MRSA infections among inmates can be made by passive or active surveillance. Waiting for inmates to access medical care for “spider bites”, rashes, bumps, or boils is passive surveillance. This is appropriate where there are very few cases of staph skin infections. Facilities with multiple cases need more active programs for recognition, including routine screening for infections and the use of diagnostic tests.
Misconceptions about the nature of MRSA skin infections may hinder early identification. For example, some inmates with MRSA have complained of having spider or insect bites, and they may not seek or receive timely treatment. This treatment delay may allow the spread of infection.
Identification of MRSA infections among inmates can be made by passive or active surveillance. Waiting for inmates to access medical care for “spider bites”, rashes, bumps, or boils is passive surveillance. This is appropriate where there are very few cases of staph skin infections. Facilities with multiple cases need more active programs for recognition, including routine screening for infections and the use of diagnostic tests.
Misconceptions about the nature of MRSA skin infections may hinder early identification. For example, some inmates with MRSA have complained of having spider or insect bites, and they may not seek or receive timely treatment. This treatment delay may allow the spread of infection.
Diagnostic Tests:
The reliability of such diagnostic methods as bacterial cultures and susceptibility testing is enhanced by supplying the healthcare staff with resources to allow adequate specimen collection for culture and by staff using the proper technique when obtaining material for culture and susceptibility testing (e.g. culturing exudate, not dry swab).
The reliability of such diagnostic methods as bacterial cultures and susceptibility testing is enhanced by supplying the healthcare staff with resources to allow adequate specimen collection for culture and by staff using the proper technique when obtaining material for culture and susceptibility testing (e.g. culturing exudate, not dry swab).
Screening:
Recognition of infections can be improved if all detainees/inmates are interviewed and given a physical examination at the following times:
Recognition of infections can be improved if all detainees/inmates are interviewed and given a physical examination at the following times:
- At intake from the community or transfer from other facilities
- When detainees/inmates complain of skin lesions
- When there has been exposure to an MRSA- infected detainee/inmate, particularly by persons who may be at high risk for MRSA infection, including those who have been recently hospitalized, have a suppressed immune system, use medical devices, such as a dialysis machine or a urinary catheter, or who have had a previous colonization with MRSA.
Treatment
Measures to ensure adequate treatment include mechanical drainage (through surgical incision), antibiotic therapy, and wound care.
Mechanical Drainage
Draining abscessed lesions is the highest priority, including incision when medically appropriate.
Wound Care
Cover each draining lesion completely with a sterile gauze dressing. Under the supervision of qualified health care staff, change dressings daily (or whenever saturated with drainage). If there will be times when there is no healthcare staff available, give extra dressing supplies and complete instructions for the dressing change to patients who have draining skin lesions. Ensure that the detainee/inmate understands how to correctly change the dressing.
Antibiotic Therapy
Reserve antibiotic therapy solely as an adjunct to drainage and wound care for local infections. Where antimicrobial use is appropriate, use antimicrobial agents that are recommended as effective against MRSA. Adjust treatment after antimicrobial susceptibility results are available; discontinue penicillins or cephalosporins if MRSA is confirmed by culture. When skin lesions appear actively infected at the end of treatment, re-evaluate the patient to assess the need for continuation of antibiotics, for repeat incision and drainage, or for decolonization of nasal carriers. While they are on therapy, monitor the patient for side effects and non-adherence to antibiotic therapy.
Measures to ensure adequate treatment include mechanical drainage (through surgical incision), antibiotic therapy, and wound care.
Mechanical Drainage
Draining abscessed lesions is the highest priority, including incision when medically appropriate.
Wound Care
Cover each draining lesion completely with a sterile gauze dressing. Under the supervision of qualified health care staff, change dressings daily (or whenever saturated with drainage). If there will be times when there is no healthcare staff available, give extra dressing supplies and complete instructions for the dressing change to patients who have draining skin lesions. Ensure that the detainee/inmate understands how to correctly change the dressing.
Antibiotic Therapy
Reserve antibiotic therapy solely as an adjunct to drainage and wound care for local infections. Where antimicrobial use is appropriate, use antimicrobial agents that are recommended as effective against MRSA. Adjust treatment after antimicrobial susceptibility results are available; discontinue penicillins or cephalosporins if MRSA is confirmed by culture. When skin lesions appear actively infected at the end of treatment, re-evaluate the patient to assess the need for continuation of antibiotics, for repeat incision and drainage, or for decolonization of nasal carriers. While they are on therapy, monitor the patient for side effects and non-adherence to antibiotic therapy.
Prevention of Transmission
Jail and prison environments are conducive to the spread of MRSA. The following conditions contribute to the continued spread of MRSA among inmates:
- Antibiotic pressure (the effect of indiscriminate use of antibiotics)
- Sub-optimal personal hygiene
- Sub-optimal laundering of underclothing and towels
- Sub-optimal environmental cleaning
A number of correctional systems have worked successfully with state and local health departments to address the spread of MRSA in correctional facilities. The following is a compilation of case identification, treatment and prevention strategies implemented by these institutions. The feasibility of these strategies will vary by facility, the regulations of individual institutions, and the nature of the participation by local health authorities in managing outbreaks. The most important aspects of preventing transmission of MRSA in correctional facilities include personal hygiene, environmental cleaning, use of standard precautions by all facility personnel and staff and detainee/inmate education.
Personal Hygiene for Detainees/ Inmates
Correctional staff should:
Encourage daily showering with soap and water
Allow access to antibacterial soap, sinks, and towels (the latter laundered regularly)
Consider the use of alcohol- based hand sanitizers during an outbreak
Encourage daily showering with soap and water
Allow access to antibacterial soap, sinks, and towels (the latter laundered regularly)
Consider the use of alcohol- based hand sanitizers during an outbreak
Detainees and inmates should:
Avoid touching lesions, drainage, or wound dressings of infected patients
Practice hand hygiene if contact occurs with lesions, drainage, or dressings
Avoid the sharing of personal items
Avoid touching lesions, drainage, or wound dressings of infected patients
Practice hand hygiene if contact occurs with lesions, drainage, or dressings
Avoid the sharing of personal items
Environmental Cleaning of Cell Housing
Regularly clean or properly dispose of medical equipment used to care for MRSA-infected patients. Dispose of dressings in compliance with state and local regulations. A hospital-grade disinfectant-detergent registered by the EPA should be used according to manufacturer’s instructions for the daily cleaning of environmental surfaces, including sinks, showers, and toilets. A bleach solution is acceptable for this cleaning. Take care to ensure that bleach solutions are appropriately diluted (1:100 dilution of concentrated bleach) and changed when dirty. Using hot water (>160℉ for 25 minutes) or bleach, properly launder clothing and linens. Dry clothes completely before they are removed from the dryer. Ensure that detainees/inmates receive at least two changes of linens per week, daily exchanges of underwear, and a twice-weekly change of outer clothing.
Standard Precautions for Correctional Facility Personnel
Practice adequate hand hygiene before and after contact with blood, body fluids, or other possibly contaminated surfaces.
Wash hands between patient contacts.
Wear gloves when in contact with blood, body fluids, or other possibly contaminated surfaces.
Change gloves between different tasks and remove gloves, followed by hand hygiene, promptly after use.
Mask and protect the eyes whenever splashing of body fluids is likely.
Gown whenever personal clothing could become soiled with body fluids.
When possible, notify other facilities and health departments when transferring or releasing patients with MRSA infection.
Assign single cell housing to an infected patient, or cohort with other MRSA-infected patients. Consider changes in work assignments for MRSA-infected patients with poor hygiene or when inadequate hygiene is prevalent, and develop a standard procedure for releasing infected patients from assignment or cohort housing.
Reserve the practice of decolonizing nasal carriers for relapsing or recurrent infections.
Wash hands between patient contacts.
Wear gloves when in contact with blood, body fluids, or other possibly contaminated surfaces.
Change gloves between different tasks and remove gloves, followed by hand hygiene, promptly after use.
Mask and protect the eyes whenever splashing of body fluids is likely.
Gown whenever personal clothing could become soiled with body fluids.
When possible, notify other facilities and health departments when transferring or releasing patients with MRSA infection.
Assign single cell housing to an infected patient, or cohort with other MRSA-infected patients. Consider changes in work assignments for MRSA-infected patients with poor hygiene or when inadequate hygiene is prevalent, and develop a standard procedure for releasing infected patients from assignment or cohort housing.
Reserve the practice of decolonizing nasal carriers for relapsing or recurrent infections.
Education
Develop a comprehensive program to:
Educate detainees/inmates, personnel, and visitors about MRSA
Emphasize good personal hygiene practices
Discuss the most important causes of disease transmission, such as manipulation of draining wounds that can result in hand-to-hand spread
Facilitate rapid recognition of skin lesions consistent with S. aureus infection
Focus work-specific infection control education to particular groups of personnel and detainees/ inmates, including those that work in laundry service, housekeeping, food service, and health care.
Emphasize good personal hygiene practices
Discuss the most important causes of disease transmission, such as manipulation of draining wounds that can result in hand-to-hand spread
Facilitate rapid recognition of skin lesions consistent with S. aureus infection
Focus work-specific infection control education to particular groups of personnel and detainees/ inmates, including those that work in laundry service, housekeeping, food service, and health care.
Barriers to Implementation of Prevention Measures
Certain barriers unique to correctional facilities may pose challenges for the prevention and control of MRSA, particularly when rapid intervention is required following a cluster of MRSA cases. Access to health care, infection control, monitoring, and community awareness have been recurrent issues in the investigation of past outbreaks.
Healthcare Access Barriers
Required co-payment to see a practitioner for skin infections.
Limited hours of physician or mid-level practitioners, or other rules inhibiting access to the facility clinic.
Unavailability of security and transportation when an outside healthcare resource is required.
Community Awareness
Inadequate recognition among lay people that boils and skin infections can be transmitted from person to person.
Insufficient knowledge that this transmission can be prevented.
Monitoring Barriers
Inadequate surveillance for new infections because of lack of resources and the complexity of the task in the correctional facility system.
Lack of continuity of care after diagnosis of infection because of frequent movement of detainees/inmates inside or outside the facility.
Insufficient information from local health departments regarding MRSA outbreaks in the community.
MRSA Pocket Guide, CDC, 2005
http://www.cdc.gov/mrsa/index.html

